Treating with Lymphangitis
Lymphangitis is sometimes referred to as “blood poisoning” due to the infection rapidly causing severe illness and sometimes death. It is usually caused by a bacterial infection.
The bacteria enter the body through a cut, scrape, bite or wound of some sort. If left untreated, the bacteria can spread in the skin around the area, causing cellulitis, and also rapidly spread to the bloodstream, causing sepsis.
Because it affects the lymphatic system, waste materials from nearly every organ in the body drain into the lymphatic vessels and are filtered in the lymph nodes. Foreign bodies, such as bacteria or viruses, are processed in the lymph nodes to generate an immune response to fight infection.
 Causes
Causes
Acute lymphangitis is most often caused by the bacterium Streptococcus pyogenes. This potentially dangerous bacterium also causes strep throat, infections of the heart, spinal cord, and lungs, and in the 1990s has been called the “flesh-eating bacterium.” Staphylococci bacteria may also cause lymphangitis.
Although anyone can develop lymphangitis, some people are more at risk. People who have had radical mastectomy (removal of a breast and nearby lymph nodes); a leg vein removed for coronary bypass surgery; or recurrent lymphangitis caused by tineapedis (a fungal infection on the foot), tend to be at an increased risk for lymphangitis.
Other conditions that increase your risk of lymphangitis include:
• diabetes
• immunodeficiency (loss of immune function)
• chronic steroid use
• varicella (chicken pox).
Symptoms
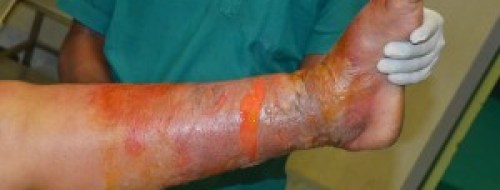
The characteristic symptoms of acute lymphangitis are the wide, red streaks which travel from the site of infection to the armpit or groin. The affected areas are red, swollen, and painful. Blistering of the affected skin may occur. The bacterial infection causes a fever of 100-104°F (38-40°C).
Other symptoms that may be experienced include:
• general ill feeling
• muscle aches
• chills
• loss of appetite
• headache
• aching muscles.
Diagnosis
If lymphangitis is suspected, the person should call his or her doctor immediately or go to an emergency room. Acute lymphangitis could be diagnosed by the family doctor, infectious disease specialist, or an emergency room doctor, since painful, red streaks just below the skin surface and the high fever are symptomatic of it. A sample of blood would be taken for culture to determine whether the bacteria have entered the bloodstream. A biopsy (removal of a piece of infected tissue) sample may be taken for culture to identify which type of bacteria is causing the infection. Diagnosis is immediate because it is based primarily on the symptoms. Most insurance policies should cover the expenses for the diagnosis and treatment of acute lymphangitis.
 Treatment
Treatment
Because of the serious nature of this infection, treatment would begin immediately, even before the bacterial culture results were available. The only treatment for acute lymphangitis is to give very large doses of an antibiotic, usually penicillin, through the vein. Growing streptococcal bacteria are usually eliminated rapidly and easily by penicillin. The antibiotic clindamycin may be included in the treatment to kill any streptococci which are not growing and are in a resting state. Alternatively, a “broad spectrum” antibiotic may be used which would kill many different kinds of bacteria.
Besides the antibiotics your health care provider may also prescribe:
• pain medication
• anti-inflammatory medication, to reduce swelling
• surgery, to drain any abscesses that may have formed
• intravenous (IV) antimicrobial therapy, antibiotics given directly into the veins.
You can aid healing and ease pain by applying a hot compress at home. Run hot water over a washcloth or towel and apply it to the tender area. Apply three times a day. The warmth will promote blood flow and encourage healing. You can also do this by taking a warm shower and placing the shower-head over the infected area. If possible, keep the infected area elevated. This helps reduce swelling and slows the spread of infection.
Prognosis
Complete recovery is expected if antibiotic treatment is begun at an early stage of the infection. However, if untreated, it can spread, causing tissue damage. Extensive tissue damage would need to be repaired by plastic surgery. Spread of the infection into the bloodstream could be fatal.
Prevention
Lymphangitis is very difficult to prevent, because it can represent a normal reaction to infection. However, it may be prevented by treating skin infections early, including:
• Avoiding injury to the skin
• Avoiding insect bites
• Avoiding scratching your skin
• Skin ulcer treatment
• Appropriate wound care.

 WhatsApp us!
WhatsApp us!